Osteoporosis, often referred to as the “silent disease,” is a common yet underdiagnosed condition that weakens bones, making them fragile and more prone to fractures. Among the various types of fractures that can result from osteoporosis, spinal fractures, also known as vertebral compression fractures, are particularly significant. In this blog, we will delve into the connection between osteoporosis and spinal fractures, exploring the causes, consequences, prevention, and treatment options for individuals at risk of or affected by these debilitating conditions.
Understanding Osteoporosis
Osteoporosis is a condition characterized by a reduction in bone density and quality, leading to bones becoming fragile and susceptible to fractures. This weakening of the bones occurs when the body loses bone mass more rapidly than it can replace it. Although osteoporosis can affect any bone in the body, it most commonly manifests in the hip, spine, and wrist.
The Link between Osteoporosis and Spinal Fractures
Spinal fractures are often the result of weakened vertebrae, which can no longer support the body’s weight effectively. These fractures can occur due to minor trauma or even as a result of routine activities like bending or lifting. The link between osteoporosis and spinal fractures lies in the deterioration of bone density and strength caused by osteoporosis.
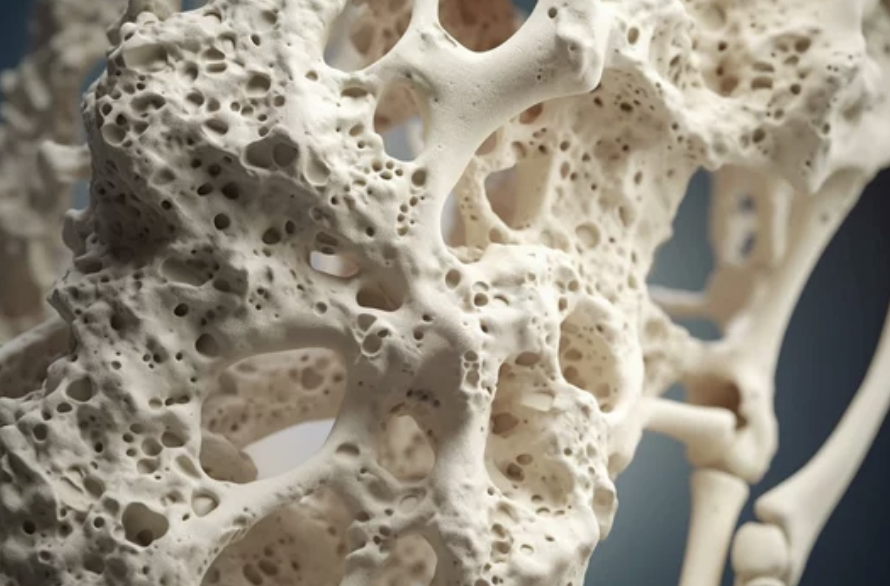
When osteoporosis progresses, it significantly compromises the structural integrity of the spine. The vertebrae in the spine become porous and less dense, resembling a honeycomb-like structure. This reduction in bone density weakens the spine, making it vulnerable to fractures. Spinal fractures typically occur in the thoracic and lumbar regions of the spine and can lead to pain, deformity, and a decreased quality of life.
The Consequences of Spinal Fractures
Spinal fractures can have a profound impact on an individual’s physical and emotional well-being. Some common consequences of these fractures include:
- Chronic Pain: Spinal fractures often lead to chronic back pain, which can be debilitating and challenging to manage.
- Loss of Height: Vertebral compression fractures can cause a noticeable loss in height as the spine becomes compressed and the person’s posture changes.
- Reduced Mobility: Mobility can be severely affected due to pain and changes in posture, making it difficult to perform everyday activities.
- Decreased Quality of Life: Chronic pain and reduced mobility can lead to depression, anxiety, and a lower overall quality of life.
- Increased Risk of Future Fractures: Once a spinal fracture occurs, the risk of future fractures in the spine and other bones increases substantially.
Preventing Osteoporosis and Spinal Fractures
Prevention is the key to avoiding the devastating effects of osteoporosis and spinal fractures. Here are some strategies to reduce the risk:
- Healthy Diet: Adequate intake of calcium and vitamin D is crucial for maintaining bone health. Include dairy products, leafy greens, and fortified foods in your diet.
- Regular Exercise: Weight-bearing exercises like walking, dancing, and weightlifting can help strengthen bones and improve balance.
- Lifestyle Modifications: Avoid smoking and excessive alcohol consumption, as these habits can weaken bones.
- Medications: In some cases, healthcare providers may prescribe medications specifically designed to increase bone density and reduce fracture risk.
- Bone Density Testing: Regular bone density scans, such as Dual-Energy X-ray Absorptiometry (DEXA) scans, can help assess bone health and determine the need for treatment.
Treatment Options
For individuals already diagnosed with osteoporosis or those who have experienced spinal fractures, several treatment options are available:
- Medications: Medications like bisphosphonates, denosumab, and parathyroid hormone analogs can help increase bone density and reduce the risk of fractures.
- Pain Management: Managing pain through medications, physical therapy, and lifestyle modifications can improve overall comfort and functionality.
- Vertebroplasty and Kyphoplasty: These minimally invasive procedures involve injecting bone cement into the fractured vertebrae to stabilize them and alleviate pain.
- Bracing: Customized braces can help support the spine and improve posture.
Conclusion
Osteoporosis and spinal fractures are closely connected, with the former significantly increasing the risk of the latter. Understanding this relationship is vital for early diagnosis, prevention, and effective management of these conditions. By adopting a proactive approach to bone health through a healthy lifestyle, regular check-ups, and appropriate treatments, individuals can reduce their risk of spinal fractures and enjoy a higher quality of life as they age. It’s crucial to remember that osteoporosis is not an inevitable part of aging, and with the right measures, we can all take steps to maintain strong and healthy bones throughout our lives.